What is breast engorgement?
What complications can arise from breast engorgement?
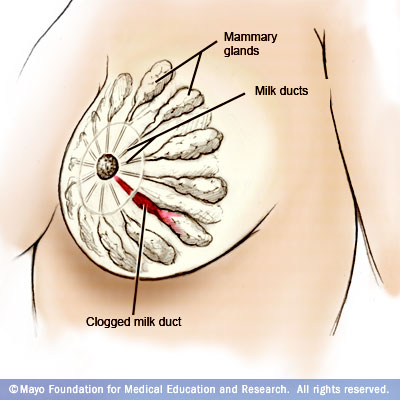
Besides being very uncomfortable, engorgement can lead to clogged ducts. A clogged duct is a milk duct that has become blocked in some way generally by the swollen tissues surrounding it. When a milk duct becomes clogged a hard, painful lump will appear on the breast. Clogged ducts can occur with or without engorgement. Due to the swelling and inflammation, clogged ducts generally go hand-in-hand with engorgement if the issue is not quickly resolved.
If a clogged duct is not properly released and drained it can soon lead to a very serious infection called mastitis. Mastitis can cause; fever, chills, a warm or 'hot' spot, redness of the breast tissue, and can be extremely painful. It is very important if you experience any of these symptoms or suspect an infection that you contact your care provider immediately so you can be assessed and placed on antibiotics that are safe for breastfeeding. If not treated appropriately, mastitis can turn into a breast abscess that must be surgically drained.
Engorgement also poses nursing challenges. Due to the swelling and inflammation of the breasts the nipple and areola may change shape or become very hard. This can make it difficult or impossible for a baby to latch and nurse effectively. A poor, ineffective latch can cause damage to the nipple, pain when nursing above and beyond what is already being experienced with engorgement, and frustration from the baby as they are not able to get an adequate supply of milk. A poor latch also means that the baby is unable to express and empty the breast fully during a feeding leading to more engorgement, clogged ducts, and possibly result in diminished milk supply.
How do you resolve breast engorgement?
The best way to resolve engorgement is to empty and soften the breast by nursing, pumping or manually expressing your breastmilk. Nursing frequently and on-demand can help resolve moderate engorgement fairly quickly. If the engorgement is moderate or the baby is having trouble latching, manually expressing some milk into a towel or a burp cloth, will help to soften the areola and nipple area. If you are exclusively pumping, simply try pumping more often. You should be pumping as frequently as your baby would be nursing, so every two to four hours within the first few weeks of life.
Any clogged ducts need to be broken up and released as well. If you are nursing, position your baby's chin towards the duct. This allows them to help unclog the duct by using the suction created during nursing. While your baby is latched and actively nursing, use the ball of your thumb to massage or rub the lump. This can be painful but it is important to stick with it and go until the duct is clear. This should be done while you are pumping or manually expressing your milk as well.
If your engorgement is due to weaning, or because you are suppressing lactation, do not fully empty the breast when manually expressing or pumping. Milk production is a supply and demand system, so the more you empty your breasts the more milk your body will make. Just express enough milk to soften the breast tissue a bit and relive the pressure. If you are weaning and you decided to go cold turkey, it may be beneficial to consider weaning down over a few days vs stopping all together if that is an option. Just decrease the length and amount of nursings daily and watch for engorgement.
Here are some tips and techniques to try to help soothe engorged breasts and achieve a better latch:
1. Choose The Right Bra
A tight or ill-fitted bra with an underwire may be exacerbating the issue. Find a comfortable nursing bra that provides support without being too snug, preferably without an underwire.
2. Cabbage Leaves
3. Epsom Salts
Some lactation consultants recommend soaking the breasts in a warm water and epsom salt solution to help provide relief. You can use a basin, sink or anything deep enough for you to be able to fully submerge your breasts. Fill with warm water and add one to two handfuls of Epsom Salts. Do not use salts that have essential oils or fragrances added to them as these can be too strong to expose your newborn to. Submerge and soak your breasts until the water cools or for five to ten minutes. If you have cracked or bleeding nipples, apply a thin coat of lanolin over them before submerging the breasts so that it does not sting. After soaking, rinse breasts with cool, clean water. You can soak your breasts before each feeding or as often as you wish during the day for up to three days. Most women feel relief within 24 hours of treating with Epsom Salts.
4. Manual Expression/Pumping
While you do not want to express or pump your breasts so frequently or fully that you end up increasing your supply unintentionally, expressing enough milk to soften your nipple or your breast tissue will not only relieve some of the discomfort of engorgement but also allow your baby to achieve a better and more efficient latch. This could also help if you have a very forceful let down that causes your baby to choke, sputter, or unlatch and become fussy at the breast. Keep a small washcloth, towel or burp cloth handy to express your milk into right before latching your baby if you are manually expressing. Alternatively, you can use a clean container or bottle to catch and store any expressed milk for later. This video published by Stanford Medicine with material developed by Jane Morton, M.D. demonstrates an excellent method for hand expressing breastmilk.
5. Reverse Pressure Softening
If your nipple and areola have become so flat or hard that your baby is unable to latch or is struggling to achieve a good latch, reverse pressure softening can help resolve that issue. First, wash your hands as you are going to want to nurse immediately following this technique. With one hand, gently cup the underside of your breast. Using two fingers on your free hand, apply steady, firm pressure on the areola right by the nipple. Hold for five to ten seconds and then release. Repeat in a circular motion around the nipple until the areola is softened. The following short video created by LittleBearLactation shows how to perform this technique.
Little Bear Lactation, "Relieving Breast Pressure With Reverse Pressure Softening", YouTube, September 28, 2018, youtube.com/watch?v=NMzR_X13Mc8
If you have tried the techniques listed above but are still experiencing engorgement issues or suspect your baby is not latching correctly due to fussiness or your breasts not being fully expressed during feedings, please contact a lactation consultant to evaluate you.
How do you resolve engorgement while suppressing lactation?
If you are trying to suppress lactation altogether, wear a firm, supportive bra or bind your breasts with a wide, soft ace bandage. Keeping them compressed will help them to produce less milk and will also keep milk production from being stimulated by touch or movement. Keeping cool cabbage leaves on your breasts may help to relieve your engorgement and can help diminish your supply faster. Ice or cold gel packs placed in your bra can also provide relief from pain and swelling. You may have to manually express very small amounts of milk, just enough to soften the breast and keep lumps from forming, when in the shower or if your breasts become very swollen, hard or lumpy. Remember that your milk production is a supply and demand system so if you fully empty your breasts or go beyond expressing just enough to relieve some pressure your body will likely increase its production. Avoid soaking your breasts in warm water, such as in the tub, or prolonged spray from a hot shower as heat can stimulate milk production. Keep a close eye on possible clogged ducts or mastitis and tell your care provider right away if you develop a fever, redness or signs of infection.
Breastfeeding Resources:
Kellymom.com provides evidence-based research and information regarding breastfeeding and lactation.
ibconline.ca provides educational videos, guidance, information and support for breastfeeding developed by Dr. Jack Newman, a physician specializing in breastfeeding support and advocacy.
Le Leche League U.S.A. provides information and support for breastfeeding families. Click on the link for more information or to find a local LLL group near you.
Recommended Reading:
Dr. Jack Newman's Guide To Breastfeeding, Dr. Jack Newman & Teresa Pitman
The Nursing Mother's Companion - 7th Edition, Kathleen Huggins, R.N., M.S.
Follow me on Facebook!
Questions about pregnancy, birth or postpartum life?
Interested in hiring a doula?
Please feel free to contact me
or check out my website!
No comments:
Post a Comment