What is folate acid?
Folate acid is a B-vitamin (B9) that can be found naturally in many food sources. Folate acid is readily converted into it's activated form, L-methylfolate or methyltetrahydrofolate (MTHF), in the digestive system prior to entering your bloodstream. L-methylfolate is required to make DNA and other genetic material. It also plays a role in creating red blood cells, building your immune system and maintaining good mental health.
What is folic acid?
Folic acid is the synthetic version of folate acid. It is almost identical molecularly to folate acid and was once believed to be metabolized more efficiently in our bodies than it's naturally occurring counterpart. However we now know that unlike folate acid which easily converts into L-methyfolate, folic acid is metabolized by the liver and goes through a lengthy process to complete its full conversion. This biological process is inefficient and has been linked to certain health issues.
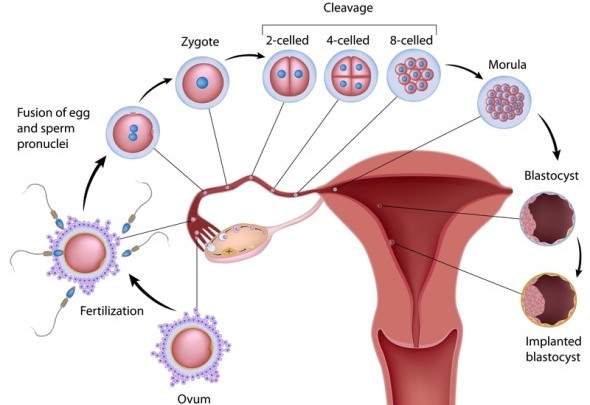
What role does folate acid play in fetal development?
Folate acid is vital in the development of your baby's nervous system, especially during the formation of the neural tube. This tube is the building block for your baby's spinal cord and brain. Folate acid is so important for fetal development that women who are planning on or actively trying to become pregnant should also be taking a folate supplement. This is critical because neural tube defects occur between the third and fourth week of pregnancy which is well before most women even know they are pregnant*. Taking the minimum of between 400 and 800 micrograms (mcg) of folate acid daily prior to conception helps eliminate the risk for neural tube defects.
In 1996 the United States passed a law mandating that certain grain and cereal products (like bread) be fortified with folic acid. This was to ensure that women of childbearing age where meeting minimum daily requirements of folate and reduce the instances of neural tube defects as many women are unaware of the importance of taking folate acid prior to conception. Even with these fortified foods, women routinely do not get the amount of folate needed to prevent neural tube defects without taking some form of folate acid supplement, either as a part of a prenatal vitamin or as a single supplement.
So if both folate and folic acid provide the necessary conversion to L-methylfolate, why does it matter which one to take during pregnancy?
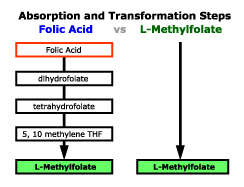 Many physicians firmly believe there is no significant difference between using a folate acid supplement vs a folic acid. In fact, since there is such a minute difference between the two many people use the terms "folic" and "folate" interchangeably, which can lead to a lot of confusion. While it is true that folic acid ultimately converts into the active form of L-methyfolate, the process it must go through is lengthy and rather inefficient. Studies have shown that even with this process there is still a detectable amount of un-metabolized folic acid left in the bloodstream, even after fasting. High levels of un-metabolized folic acid has been linked to several health concerns, including increasing your risk for cancer**.
Many physicians firmly believe there is no significant difference between using a folate acid supplement vs a folic acid. In fact, since there is such a minute difference between the two many people use the terms "folic" and "folate" interchangeably, which can lead to a lot of confusion. While it is true that folic acid ultimately converts into the active form of L-methyfolate, the process it must go through is lengthy and rather inefficient. Studies have shown that even with this process there is still a detectable amount of un-metabolized folic acid left in the bloodstream, even after fasting. High levels of un-metabolized folic acid has been linked to several health concerns, including increasing your risk for cancer**. As many as 40% of the population may also suffer from what is known as the MTHFR mutation. This mutation can halt the body's natural ability to convert folic acid into L-methylfolate. Essentially, because your body cannot convert the folic acid into its activated state it is not able to metabolize it, which can lead to deficiencies and serious health issues.
While not everyone who has the MTFHR mutation suffer from its possible health issues, some health practitioners recommend genetic testing for this mutation if you have suffered multiple miscarriages as this gene mutation and the subsequent vitamin deficiency may be the root cause.
It is important to remember that if you are not metabolizing all of the folic acid you are taking, whether due to its inefficient metabolic processing or a genetic mutation, your developing baby is not benefiting from it either.
How do I ensure that I am taking a more readily usable form of folate?
Besides eating foods high in folate like spinach, avocados, asparagus and broccoli, you want to find a prenatal vitamin or a folate acid supplement that has an activated form listed as an active ingredient. The following are a few of the activated forms of folate/folic acid that do not need to go through any conversion process in the body***:
- L forms
- 6(s) forms
- Quatrefolic
- L-methylfolate Calcium
How do I find a good prenatal vitamin with folate acid vs folic acid?
There are many good prenatal vitamins available on the market today. Frustratingly, the majority of them use folic acid rather than a form of activated folate acid. Fortunately there are a few brands that use the activated form, and more and more are becoming available as people become aware of the difference between the two. A quick search online can provide you with a variety of options that suit your individual preferences and nutritional needs. You can also take a stand-alone folate acid supplement along with a prenatal that does not have folic or folate acid as an active ingredient.
Whatever method you ultimately decide on, DO NOT wait until you are pregnant to start a good prenatal vitamin with folate/folic acid of some form. If you are trying to conceive, or think you may already be pregnant, now is the time to start taking care of your body and your health in order to give your baby the best prenatal nutrition.
**Cancer incidence and mortality after treatment with folic acid and vitamin B12; Ebbing M, Bønaa KH, Nygård O, Arnesen E, Ueland PM, Nordrehaug JE, Rasmussen K, Njølstad I, Refsum H, Nilsen DW, Tverdal A, Meyer K, Vollset SE.
***For a more complete list, information and comprehensive video explaining the different types of folate and folic acid, please check out this article written by Dr. Ben Lynch, mthfr.net/l-methylfolate-methylfolate-5-mthf/2012/04/05/. Dr. Lynch's site also provides in depth information regarding the MTHFR mutation as well as information pertaining to folic acid and pregnancy.
***For a more complete list, information and comprehensive video explaining the different types of folate and folic acid, please check out this article written by Dr. Ben Lynch, mthfr.net/l-methylfolate-methylfolate-5-mthf/2012/04/05/. Dr. Lynch's site also provides in depth information regarding the MTHFR mutation as well as information pertaining to folic acid and pregnancy.
Suggested Supplements:
Here are a few of the prenatal vitamins I have found that have the activated type of folate/folic acid and also adequate amounts of the other vitamins and minerals recommended for pregnancy. Always talk to your care provider about questions regarding your unique needs and requirements before starting a new supplement if you are currently pregnant or have health concerns.
- Isotonix Prenatal Activated Multivitamin - I personally have used and recommend this prenatal. It comes in a powdered form that is added to water. This helps the formula reach the same pH as your body's fluids. I especially like that it is in liquid form when you ingest it vs a big pill, which eliminates the need for binders and fillers. This also ensures optimal absorption of the ingredients so I feel you are getting a bigger bang for your buck (why pay for nutrition you aren't actually absorbing?). You can connect with Julia, who is a distributer, for more information regarding this product here.
- Seeking Health Optimal Prenatal - This pill does not have any iron added to it and so may be gentler on the gut for those who are sensitive to it. However, iron is very important to create the extra red blood cells you need to support your baby and the placenta as well as help limit postpartum bleeding. Talk to your doctor about how much iron you need in your diet and whether or not you need to supplement with an additional iron tablet to maintain a healthy pregnancy.
- Smartypants Prenatal Complete - This gummy contains Omega-3 fatty acid, DHA, and EPA sourced from small fish (indicating fish types that may be lower in heavy metals) and does not contain any iron (which may be gentler for those who are sensitive to it). Please talk to your doctor about how much iron you need in your diet to maintain a healthy pregnancy and whether or not you need to supplement with an additional iron tablet.
Follow me on Facebook!
Questions about pregnancy, birth or postpartum life?
Interested in hiring a doula?
Please feel free to contact me
or check out my website!